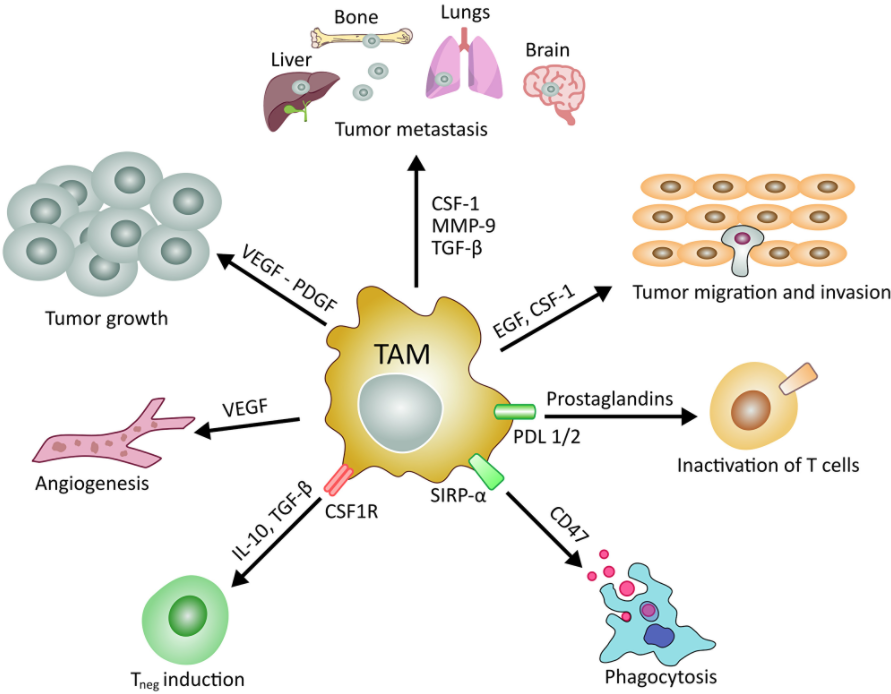
“Treg play a deleterious role in the tumor microenvironment by suppressing anti-tumor effector T cells.”
Cancer is a disease caused by the uncontrolled growth of cells that escape the body’s natural defenses. One way cancer protects itself is by taking advantage of certain immune cells called regulatory T cells, or Tregs. Normally, Tregs help prevent autoimmune diseases by controlling the immune system. But inside tumors, they behave differently. Instead of defending the body, they suppress the immune cells that could attack the cancer.
Many cancer treatments aim to activate the immune system to fight tumors more effectively. However, the presence of Tregs within the tumor makes this difficult. These cells act like bodyguards for the cancer, blocking the immune response that might otherwise slow or stop tumor growth.
Researchers have tried to eliminate Tregs by targeting a protein called CD25, found on their surface. However, earlier efforts often failed because these treatments also interfere with interleukin-2 (IL-2), a molecule that is essential for other immune cells to function. Blocking IL-2 weakens the entire immune response, limiting the treatment’s effectiveness.
To overcome this challenge, scientists recently developed a new antibody called 2B010. This study, titled “A novel anti-human CD25 mAb with preferential reactivity to activated T regulatory cells depletes them from the tumor microenvironment,” was published in Oncotarget (Volume 16)
The Study: Finding a New Antibody Against Tumor Tregs
To develop a more selective tool for targeting Tregs, researchers from the National Institute of Allergy and Infectious Diseases, in collaboration with Boehringer Ingelheim and led by Maja Buszko and Ethan M. Shevach, conducted an experiment using mice. The animals were exposed to human regulatory T cells that had been activated and expanded in the laboratory. This exposure triggered the mice’s immune systems to produce antibodies against the Tregs. Among the resulting hybridomas, one named 2B010 stood out for producing an antibody capable of binding to CD25, a protein commonly found on the surface of active Tregs.
The Results: 2B010 Shows Selective Treg Depletion and Immune Activation
The 2B010 antibody was effective in both cell-based and animal studies. It was able to detect and remove regulatory T cells that were actively protecting tumors, without disrupting IL-2 signaling. This allowed the rest of the immune system to stay functional.
In a mouse model of human breast cancer, treatment with 2B010 significantly reduced the number of Tregs inside the tumors. As a result, CD8+ T cells, which are responsible for killing cancer cells, became more active. While the tumors themselves did not shrink, the immune system clearly showed signs of stronger activity against the cancer.
What makes 2B010 different is its ability to distinguish between harmful and helpful immune cells. Although many immune cells express CD25 when activated, 2B010 preferentially binds to highly active Tregs within the tumor. This selectivity allows it to target only the cells that shield tumors, while sparing other important parts of the immune system.
The effect of 2B010 was not limited to the tumor site. Increased immune activity was also observed in the spleen, suggesting that this antibody may help support the body’s general immune response.
The Impact: Potential Role of 2B010 in Enhancing Cancer Immunotherapy
This discovery offers a potential direction for advancing cancer treatment. By removing the regulatory T cells that shield tumors from immune attack, the 2B010 antibody could improve the effectiveness of current immunotherapies. It may be particularly valuable when used alongside checkpoint inhibitors, drugs that help lift the immune system’s natural brakes. Together, these therapies could produce a stronger, more sustained anti-tumor response.
Since high levels of Tregs are linked to poor outcomes in many types of cancer, selectively eliminating these cells may help overcome a major obstacle in immunotherapy. In addition, because 2B010 does not interfere with IL-2 signaling, it may avoid the unintended side effects seen with earlier anti-CD25 antibodies. Together, these features make it a good candidate for more precise and better-tolerated cancer treatments.
Future Perspectives and Conclusion
While the 2B010 antibody shows strong potential in preclinical studies, its performance in human patients remains to be seen. Clinical trials will be essential to assess its safety, effectiveness, and compatibility with current cancer treatments. Researchers suggest that, with further development, 2B010 may become a valuable addition to combination immunotherapy strategies in the future.
Click here to read the full research paper published by Oncotarget.
_______
Oncotarget is an open-access, peer-reviewed journal that has published primarily oncology-focused research papers since 2010. These papers are available to readers (at no cost and free of subscription barriers) in a continuous publishing format at Oncotarget.com.
Oncotarget is indexed and archived by PubMed/Medline, PubMed Central, Scopus, EMBASE, META (Chan Zuckerberg Initiative) (2018-2022), and Dimensions (Digital Science).
Click here to subscribe to Oncotarget publication updates.
For media inquiries, please contact media@impactjournals.com.