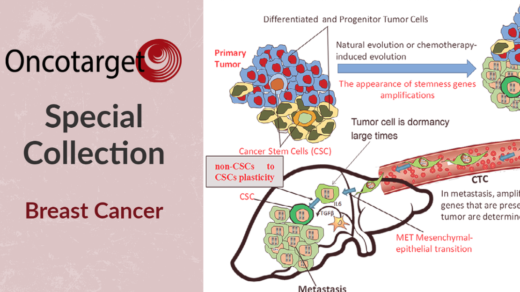
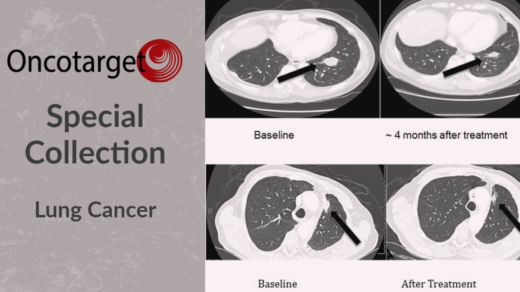
Researchers Jennifer Y. Sheng and Vered Stearns discussed the results of a study that compared weight loss interventions among overweight or obese survivors of breast cancer.

After being diagnosed with breast cancer, up to 96% of women have reported gaining weight. Medications, inactivity, food choice, and food quantity can all lead to weight gain. Studies have shown that weight gain can increase the risk of breast cancer recurrence by 40–50% and breast cancer-related mortality by 53–60%. Thus, for women with breast cancer and those who have survived breast cancer, weight management is a potentially life-saving intervention.
In an editorial paper published by Oncotarget in 2021, researchers Jennifer Y. Sheng and Vered Stearns from Johns Hopkins School of Medicine and the Johns Hopkins Sidney Kimmel Comprehensive Cancer Center discussed the results of the 2020 POWER-Remote Trial—a study among breast cancer survivors on the results of a remote-based weight loss program compared with a self-directed approach. Their editorial paper is entitled, “Innovating and expanding weight loss strategies for breast cancer survivors.”
The POWER Intervention
The Practice-based Opportunities for Weight Reduction (POWER) intervention is a 12-week behavioral weight loss program designed for overweight and obese participants. The POWER program strategy focuses on physical activity and behavioral changes, nutrition education and setting individual goals. Researchers developed the POWER-remote intervention to enable participants to engage in this weight loss program remotely through weekly video conferences and phone calls. In the current editorial paper, the researchers discussed the results from a study that adapted the POWER-remote intervention for breast cancer survivors: the POWER-Remote Trial.
“The original Practice-based Opportunities for Weight Reduction (POWER) study in obese individuals with a risk for cardiovascular disease demonstrated equivalent weight loss outcomes between in-person coaching and a remote intervention [24].”
The POWER-Remote Trial
The POWER-Remote Trial was a randomized, controlled comparative effectiveness trial that evaluated the POWER-remote intervention compared to a self-directed weight loss approach among overweight or obese breast cancer survivors. Between 2013 and 2015, 87 overweight or obese women with stage 0-III breast cancer (who completed local therapy and chemotherapy) were evaluable for analysis in this study. Forty-five women were enrolled in the POWER-remote arm of the study and 42 women were enrolled in the self-directed arm.
“Our group compared the remote-based POWER intervention (telephone calls by a coach, access to online learning materials, online self-directed dietary/activity monitoring) to self-directed weight loss in overweight or obese survivors of early-stage breast cancer [25].”
Over the course of the study, the researchers found high adherence in the POWER-remote arm, with only one participant lost in follow-up. At the 12-month mark, 51% of the POWER-remote participants lost greater than or equal to 5% of their baseline body weight. Among the self-directed participants, 17% lost 5% or more of their baseline body weight. The results of this study suggest that the POWER-remote intervention is an effective weight loss strategy. It is a cost-effective, scalable and conscientious solution to assist with weight loss among many breast cancer survivors.
Conclusion
Despite the significant improvements in weight, body composition, fitness, and quality of life seen by over half of the participants in the POWER-remote arm, the researchers also pointed out a problem. The POWER-remote intervention still did not yield significant results in almost half of the other participants. Trouble sleeping was shown as a potential culprit that hindered weight loss, while many other factors inhibiting weight loss in this population are not yet fully understood.
The authors wrote that it may be necessary to further individualize or enhance the POWER intervention to achieve greater success in breast cancer survivors. They also suggested that, in some people, the POWER program may need to be augmented with pharmacological agents to aid in weight loss. In addition, the authors believe that the payer system should be reevaluated to expand coverage for obesity treatments.
“At present, I’m conducting a phase two study to determine whether an adaptor approach with pharmacotherapy can augment obesity treatment in breast cancer survivors. This study is called the A-NEW study, which stands for an Adaptive Nutrition and Exercise Weight Loss Study,” Dr. Jennifer Sheng said in a recent Behind the Study interview with Oncotarget. “We’re also looking forward to analyzing results from the COOIN study, the Cancer, Obesity, Overweight, and Insomnia study, which was led by Dr. Janelle Coughlin.”
- Author Interview: Dr. Sheng discusses the research behind the editorial
- Author Testimonial: Dr. Sheng describes the experience publishing with Oncotarget
- Behind the Study: Transcription of Dr. Sheng’s research discussion
Click here to read the full editorial paper published by Oncotarget.
ONCOTARGET VIDEOS: YouTube | LabTube | Oncotarget.com
—
Oncotarget is a unique platform designed to house scientific studies in a journal format that is available for anyone to read without a paywall making access more difficult. This means information that has the potential to benefit our societies from the inside out can be shared with friends, neighbors, colleagues, and other researchers, far and wide.
For media inquiries, please contact media@impactjournals.com.