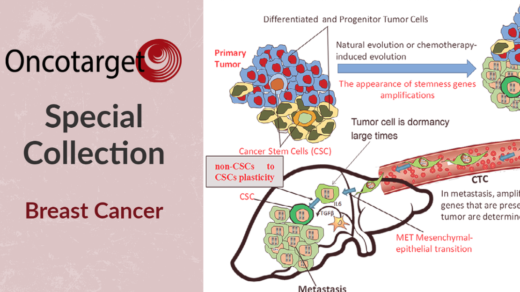
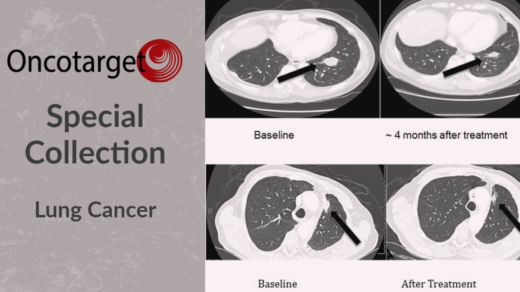
In this research perspective, researchers discuss causal and correlative approaches to identify potential biomarkers for predicting paclitaxel response.
—
Cancer therapy has come a long way from its one-size-fits-all beginning to the awakening era of personalized medicine. This change has been largely driven by the discovery of biomarkers. Biomarkers can help refine patient selection for specific therapies. A blend of causal and correlative approaches is needed to elucidate the full potential of biomarkers in cancer research. This fusion of methodologies allows for a comprehensive exploration of biomarker efficacy, leading to more accurate predictions of drug response.
In a new paper, researchers Alberto Moscona-Nissan, Karl J. Habashy, Victor A. Arrieta, Adam M. Sonabend, and Crismita Dmello from the Universidad Panamericana School of Medicine, Northwestern University and Universidad Nacional Autónoma de México discuss causal and correlative approaches to identify potential biomarkers for predicting response to paclitaxel — a commonly used chemotherapeutic agent. On February 8, 2024, their research perspective was published in Oncotarget’s Volume 15, entitled, “Combining causal and correlative approaches to discover biomarkers of response to paclitaxel.”
“[…] studying the combination of non-overlapping biomarkers’ expression, in addition to clinical and sociodemographic data could generate predictive models for paclitaxel susceptibility.”
Combining Causal and Correlative Approaches
Paclitaxel is a mainstay of treatment for various cancers, including breast, pancreatic, ovarian, and non-small cell lung carcinomas. However, the benefit derived from paclitaxel treatment varies across patients, and a significant proportion does not receive therapeutic benefit and experiences unnecessary toxicity. The variability in response to paclitaxel underscores the need for predictive biomarkers. Predictive biomarkers of response to paclitaxel can lead to improved treatment efficacy, less unnecessary toxicity, and potentially better health outcomes.
In a recent study, researchers used a whole-genome CRISPR/Cas9 knockout to identify genes that influence paclitaxel susceptibility in gliomas. They identified 51 genes that have implications in pathways such as NFkB, toll-like receptor, and MAPK signaling, transcriptional misregulation, and apoptosis. The team also identified the signal sequence receptor 3 (SSR3) gene as a predictive biomarker for paclitaxel susceptibility.
The SSR3 gene encodes the gamma subunit of the signal sequence receptor (SSR) complex, a glycosylated membrane receptor located at the endoplasmic reticulum (ER). This complex is involved in protein translocation across the ER membrane. In the study, it was found that higher SSR3 expression correlated with increased paclitaxel susceptibility in cancer cell lines. SSR3 knockout cells showed decreased susceptibility to paclitaxel, while cells overexpressing SSR3 had increased susceptibility.
The study also revealed a link between SSR3 and the unfolded protein response (UPR) pathway, which reduces the amount of unfolded proteins in the cell under stressful conditions. A positive correlation was found between SSR3 expression and IRE1a levels in glioma PDX cells. IRE1a is a serine/threonine kinase that is involved in the UPR pathway and has been implicated in various disorders.
Conclusions & Future Directions
A significant challenge in the treatment of glioblastoma is the blood-brain barrier which limits the efficacy of paclitaxel. However, innovative strategies like convection-enhanced delivery, biodegradable wafers, peptide-drug conjugates, and low-intensity pulsed ultrasound administered with microbubbles are being developed to overcome this barrier.
The researchers also wrote in their research perspective that, after identifying a potential predictive biomarker in a training cohort of patients, it is vital to validate the finding in an independent cohort. The correlation between patients’ overall survival and SSR3 expression is currently being studied in a phase 2 trial at Northwestern University. Based on the outcomes of these validations, the predictive models can be further refined by incorporating other non-overlapping histologic and molecular biomarkers along with patient demographics. The discovery of predictive biomarkers for paclitaxel response, such as SSR3, promises to significantly impact cancer treatment.
“Precision and personalized medicine can lead to a transition from a stochastic treatment response into predictable scenarios. Further identification of predictive biomarkers, validation, and study of combinations as predictive models is critical to generate a greater impact that can be translated to the bedside of patients.”
Click here to read the full research paper in Oncotarget.
—
Oncotarget is an open-access, peer-reviewed journal that has published primarily oncology-focused research papers since 2010. These papers are available to readers (at no cost and free of subscription barriers) in a continuous publishing format at Oncotarget.com.
Oncotarget is indexed and archived by PubMed/Medline, PubMed Central, Scopus, EMBASE, META (Chan Zuckerberg Initiative) (2018-2022), and Dimensions (Digital Science).
Click here to subscribe to Oncotarget publication updates.
For media inquiries, please contact media@impactjournals.com.